Benedikt Clemens, Optima team | UNAIDS uses the OPTIMA approach, which allows to optimise the allocation of resources. For instance, for Belarus the model suggested there should be higher investment on treatment (ART) and programmes for people who use drugs. Hence, Belarus modified its allocation.
Belarus then calculated expected outcomes and compared these calculations with the actual observed change. It demonstrated that the model has predictive value.
The same modelling then was use globally to estimate what would happen if investment would be scaled up? The projections suggest that in the high-coverage scenaro HIV infections and deaths would be reduced by 90% by 2020. This would mean mobilising resources from different portfolios.
The team also used modelling to estimate the results of reducing the costs (without decreasing quality) of services through the acquisition of medicines at competitive prices. The impact on health would be greatly significant without demanding an increase in expenditure.
Better allocation and better pricing can have predictable positive impacts on health and wellbeing.
Don C Des Jarlais, Mount Sinai | Complex relationship between drug use and HIV transition. Cannot expect uniform correlation between drug use of a particular drug HIV infection.
Clearly, injecting drug use has a potential impact on HIV transmission, but this is related to different aspects of use and the lives of users. So there are different ways to intervene to reduce negative effects.
Drug use networks – Different sizes, density, membership, prevalence, social norms for injecting/sexual behaviour, supplies of injection equiment and condoms; drugs used and ROA.
For stimulants, there are special issues to take into account: high frequency of injections, expectations for increased sexual pleasure, disorganised lifestyle among very heavy cocaine and ATS users, lack of scalable effective treatment.
There is a need to come up with interventions to improve health outcomes among users. Ex. suggest heavy users take ART when they’re most likely to be under the influence, because that’s when they will feel ‘normal’.
Most studies show a degree of correlations between the use of stimulant drugs (injecting cocaine, smoking crack cocaine, oral/parenteral ATS, etc.) and risk behaviour and HIV infection.
There are some successful examples of intervention efforts: Cocaine injecting HIV epidemic in Brazil (through NSP); Crack cocaine HIV epidemic in NY (through harm reduction initiatives, condom provision and increased reach of ART services). HIV infections were reduced by half or more.
We need to identify additional interventions to address specific problems in specific situations.
It might be necessary to develop interventions that do not necessarily focus on reducing use of stimulants but reducing harm.
Dr Kanna Hayashi & Dr Steven Shoptaw | Stable MMT produces reliable 3x reduction in new HIV infections. MMT also increases adherence and immune response with ART, even among homeless.
Less clear interventions for stimulants. The use of cocaine or methamphetamine among MSM does not reduce the effectiveness of ART. All people living with HIV require access to ART.
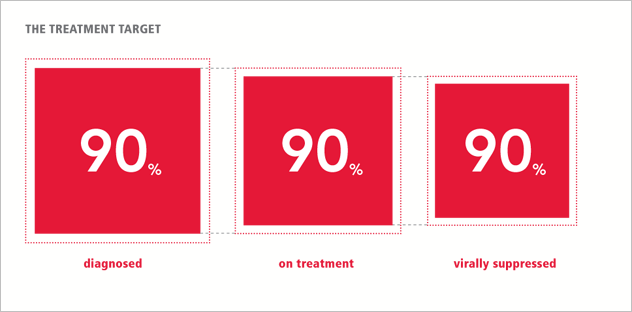
90-90-90: An ambitious treatment target to help end the AIDS epidemic.
Only 4% of PWID who are HIV+ are on ART.
Inconsistent engagement with HIV care and ART clearly poses a challenge attaining vilan suppression among PWID. Why? Which barriers? Suboptimal OST; stimulant use; social, structural and environmental factors: incarceration, stigmatisation, homelessness, socioeconomic marginalisation.
Health-focused drug policies should be based on evidence and human rights.
Drug policies need to be reoriented to focus on health and support.
Presentation of 2nd Scientific Statement Science addressing Drugs and HIV: State of the Art